If you're new to the world of hearing aids, you may be full of questions and feel overwhelmed with the myriad of choices. Which design is right for me? What's the difference between prescription and OTC hearing aids? Doing your research can help resolve some of your questions. Fortunately, we've done much of the research for you for this article!
I began practicing audiology in 1992. Over the years, I've seen thousands of patients and have actively involved myself in consumer groups for hearing loss. I wrote this guide to equip those experiencing hearing loss with the knowledge they need to find a hearing aid.
In this guide, I'll explain the different types of hearing aids that are available so you can decide which will work for you or your loved one. I'll also explain the types of hearing loss that can occur — and the early warning signs you should know.
Hearing Aid Recommendations for Every Need

- Best Hearing Aids March 17, 2026
- Best Bluetooth Hearing Aids January 28, 2026
- Best Invisible Hearing Aids January 13, 2026
- Best Over-the-Counter Hearing Aids March 10, 2026
- Best Rechargeable Hearing Aids January 28, 2026
- Best Hearing Aids for Tinnitus January 30, 2026
- Best Hearing Aids for Severe Hearing Loss January 31, 2026
- Best Behind-the-Ear Hearing Aids January 13, 2026
- Best iPhone Hearing Aids January 30, 2026
- Best Hearing Aids for Alzheimer’s Patients January 30, 2026
- Best Android-Compatible Hearing Aids January 12, 2026
- Best Hearing Aids for Single-Sided Hearing Loss January 23, 2026
- Best Hearing Aids for Active Lifestyles January 13, 2026
We’ve researched and reviewed the industry’s top providers to help you find the best hearing aid for your needs.
Hands-On Hearing Aid Reviews
- Audien Hearing Aids Review and Pricing March 14, 2026
- Beltone Hearing Aid Reviews November 24, 2025
- Eargo Hearing Aid Review November 24, 2025
- Hear.com Reviews December 9, 2025
- Jabra Enhance Hearing Aids Review March 17, 2026
- MDHearing Hearing Aids Costs and Pricing December 12, 2025
- Miracle-Ear Hearing Aid Reviews March 19, 2026
- Oticon Hearing Aid Reviews December 5, 2025
- Otofonix Hearing Aid Reviews November 21, 2025
- Phonak Hearing Aid Reviews March 19, 2026
- ReSound Hearing Aid Reviews December 8, 2025
- Rexton Hearing Aids Review November 21, 2025
- Signia Hearing Aid Reviews September 16, 2025
- Starkey Hearing Aid Reviews December 9, 2025
- Widex Hearing Aid Reviews December 9, 2025
Our detailed, hands-on reviews of the industry’s most popular hearing aids will give you an inside look at our experience with the company’s products and our key takeaways.
Hearing Aid Pricing Across the Market

- A Guide to Hearing Aid Prices February 9, 2026
- Beltone Hearing Aid Pricing November 13, 2025
- Eargo Hearing Aid Pricing September 11, 2025
- Jabra Enhance Hearing Aid Pricing February 6, 2026
- MDHearingAid Pricing December 12, 2025
- Miracle-Ear Hearing Aid Pricing October 13, 2025
- Oticon Hearing Aid Pricing February 6, 2026
- Phonak Hearing Aid Pricing December 9, 2025
- Rexton Hearing Aid Pricing December 11, 2025
- ReSound Hearing Aid Pricing November 12, 2025
- Signia Hearing Aid Pricing December 5, 2025
- Starkey Hearing Aid Pricing December 9, 2025
- Widex Hearing Aid Pricing September 15, 2025
- Zip Hearing Pricing December 11, 2025
Want a closer look at pricing and value? Visit our pricing pages for these popular providers to learn more and learn how to get the best deal on your hearing aids.
Comparing Hearing Aid Brands
- MDHearingAid vs. Eargo November 24, 2025
- Oticon vs. Beltone December 5, 2025
- Oticon vs. Starkey December 9, 2025
- Phonak vs. Beltone November 14, 2025
- Phonak vs. Oticon November 11, 2025
- Phonak vs. ReSound December 5, 2025
- Phonak vs. Signia December 8, 2025
- Phonak vs. Starkey December 9, 2025
- Phonak vs. Unitron June 24, 2025
- Phonak vs. Widex December 10, 2025
- ReSound vs. Beltone December 8, 2025
- ReSound vs. Oticon December 5, 2025
- ReSound vs. Signia December 9, 2025
- ReSound vs. Starkey December 10, 2025
- Widex vs. Oticon December 10, 2025
- Widex vs. ReSound December 5, 2025
- Widex vs. Signia December 9, 2025
- Widex vs. Starkey December 9, 2025
With so many hearing aids on the market, comparing providers side by side is a helpful way to determine which device is best for you. If you’re struggling to pick between two providers, take a look at our comparison pages.
Additional Hearing Aid Resources

- How to Pair Hearing Aids to an iPhone December 11, 2025
- How to Put in Hearing Aids December 11, 2025
- How to Use Airpods As Hearing Devices February 19, 2026
- Medicare Coverage for Hearing Aids November 24, 2025
Whether you’re looking for step-by-step how-to guides or resources on Medicare coverage for hearing aids, we’ve got you covered with a wide range of additional hearing aid resources.
I began practicing audiology in 1992. Over the years, I’ve seen thousands of patients and been actively involved in consumer groups for hearing loss. I wrote this guide to accomplish a few things.
First, I’d like more people to seek help for hearing loss. Millions of Americans (mostly seniors) have hearing loss. A discouraging fact has rung true for almost a century: just 20 percent of people who would benefit from a hearing aid wear one. In my experience, a big reason for that is a lack of knowledge. This guide aims to address this.In my experience, a big reason for this is a lack of knowledge. This guide aims to address this.
Second, I wanted to open the curtain on the seemingly endless options for hearing aids. Just like buying a car, there are hundreds of makes and models to choose from. But if you zoom out a bit, all of them have four wheels, a frame, a motor, and a body. Beyond that, most models just differ based on convenience and style. Hearing aids are much the same.
Finally, I wanted to arm you with some not-so-common tools to weed out the good, the bad, and the ugly in terms of who actually dispenses these devices. Returning to the car analogy, you want a mechanic who won’t quit “wrenching” until your ride is purring like a kitten. With a smidge of knowledge and healthy skepticism, you can push your “hearing mechanic” to help you hear the best you can.
Table of Contents
What is a Hearing Aid?
Hearing aids are electronic devices worn in or behind the ear. Hearing aids improve the lives of those with mild to significant hearing loss.
Rather, they aren't a cure for hearing loss. Rather, they improve the quality and level of sound around you. It increases your ability to comprehend human speech and enjoy the sounds of life while they're being worn. Once you pop them out, your hearing will revert to its natural state.
The moral of the story? You have to wear hearing aids to reap their benefits. That's why buying the right type is so critical. Hearing aids that don't work tend not to be worn.
How Do Hearing Aids Work?
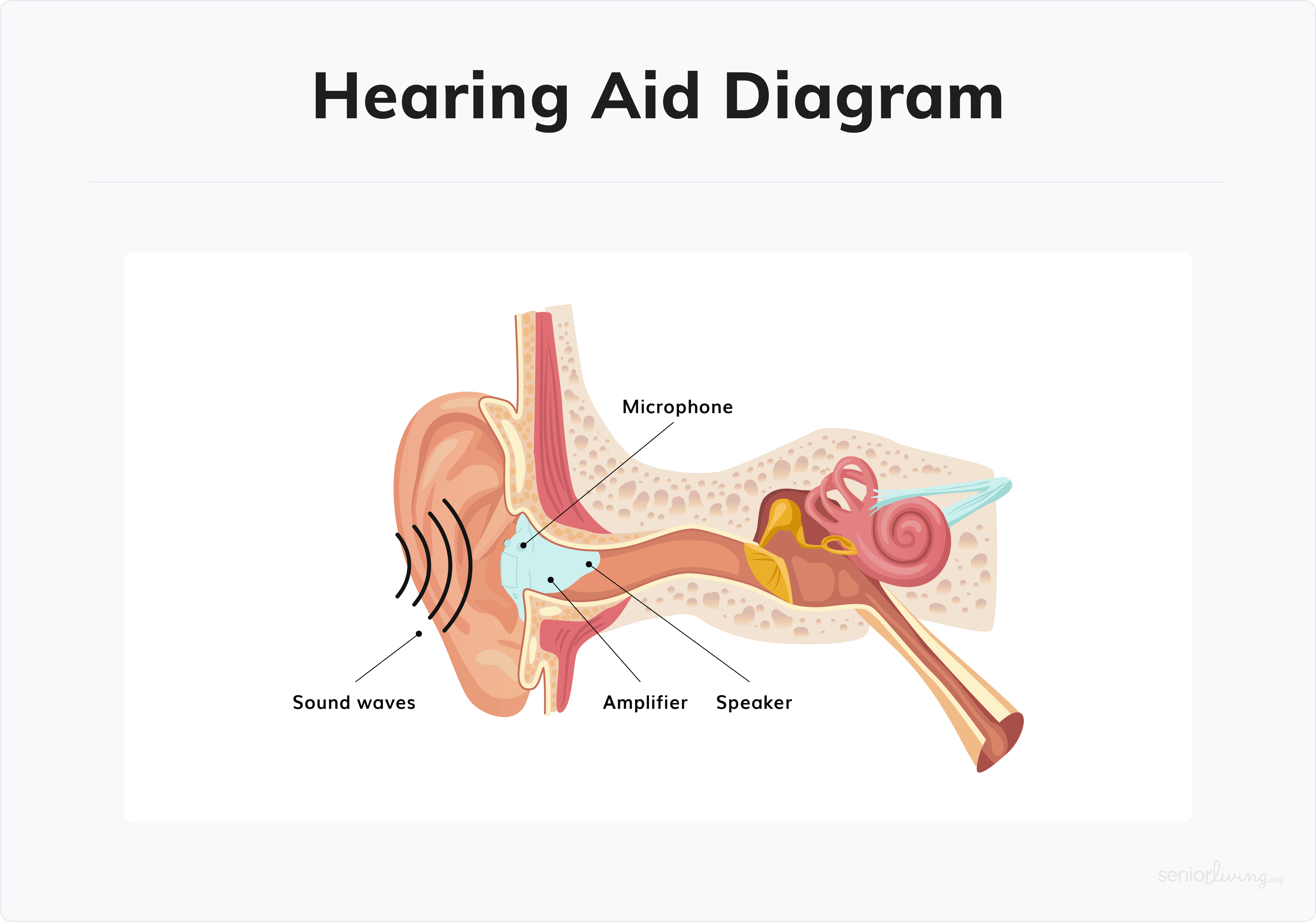
Hearing aid technology is constantly changing and improving. But in general, most hearing aids work similarly. When you wear a hearing aid, sound vibrations enter the ear and travel into the ear canal. These vibrations continue to travel through the eardrum and the small bones of the middle ear and into the inner ear. That's where the sound is processed and sent to the brain.
Hearing aids contain one or more microphones that pick up sound, a digital amplifier that makes sounds louder, and a receiver that sends sound into the ear canal. These components work together to amplify and crystalize the sounds around you. Many hearing aids are even engineered to prioritize important sounds, like voices.1
What Types of Hearing Aids Are There?
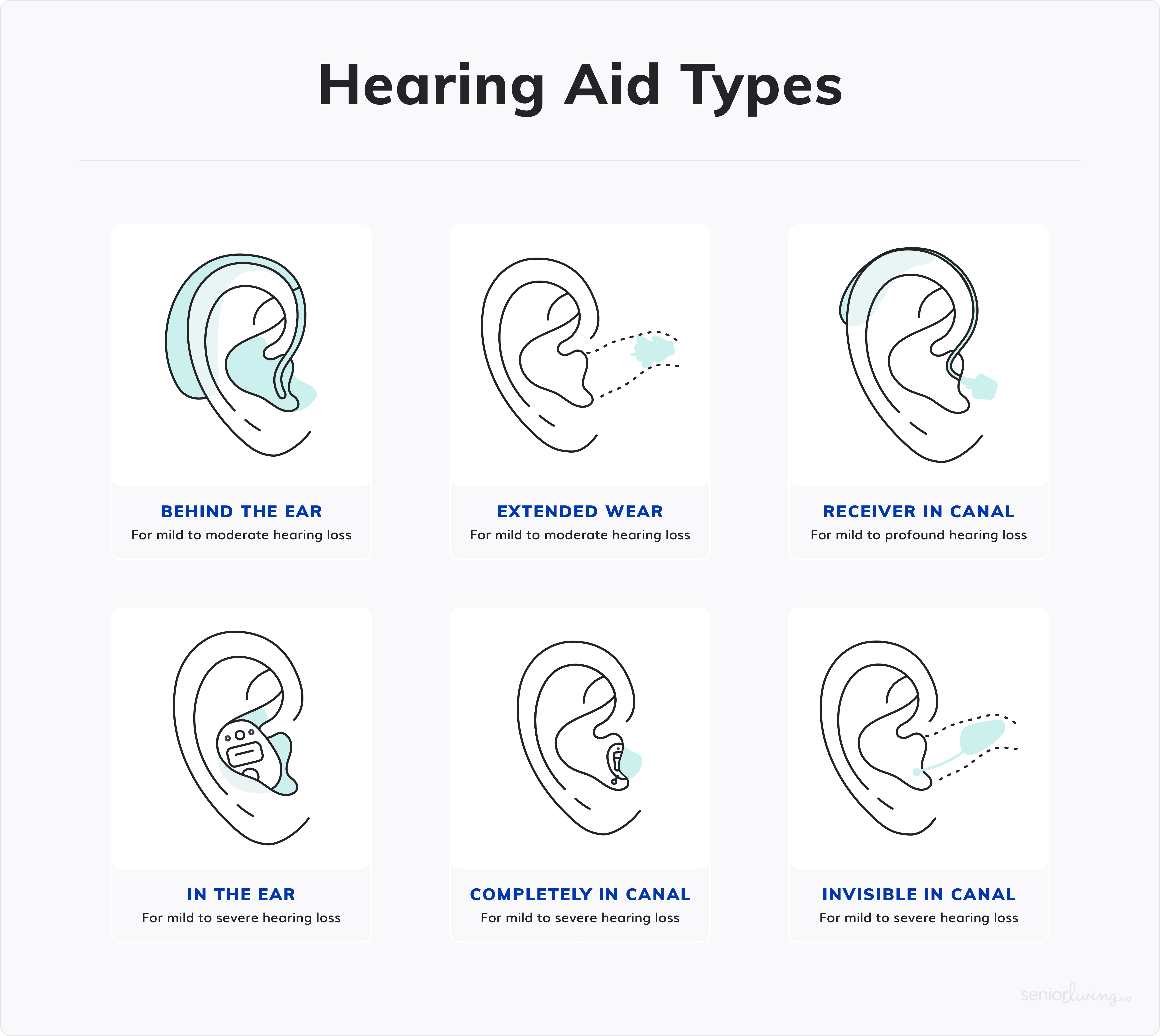
Hearing aids fall into two major categories — in-the-ear (ITE) and behind-the-ear (BTE) — and a few subcategories regarding style or shape. In general, the internal electronics are the same across styles of a given model, but some features may not be available in certain styles due to size. The currently available styles are as follows:
As you can see, there are a lot of options when it comes to the size and shape of hearing aids. As an audiologist, I've noticed that most patients prefer not to advertise their hearing loss. The exception is typically younger folks who opt for bright and noticeable BTE versions. People who prefer very discreet hearing aids should see if the invisible-in-the-canal (IIC) or extended wear (EW) options are appropriate for their hearing loss level and needs.
Unless you're completely bald, the receiver-in-canal (RIC) style is nearly invisible in most cases. That's because they can be color-matched to your hair. Hearing aids that look good (or at least acceptable) are very desirable; however, it’s essential to realize that going that small means you may have to compromise on some features.
Take a moment to check out our video on types of hearing aids below. This video covers all major hearing aid types, how they work, and some of their functionalities.
Hearing Anatomy 101
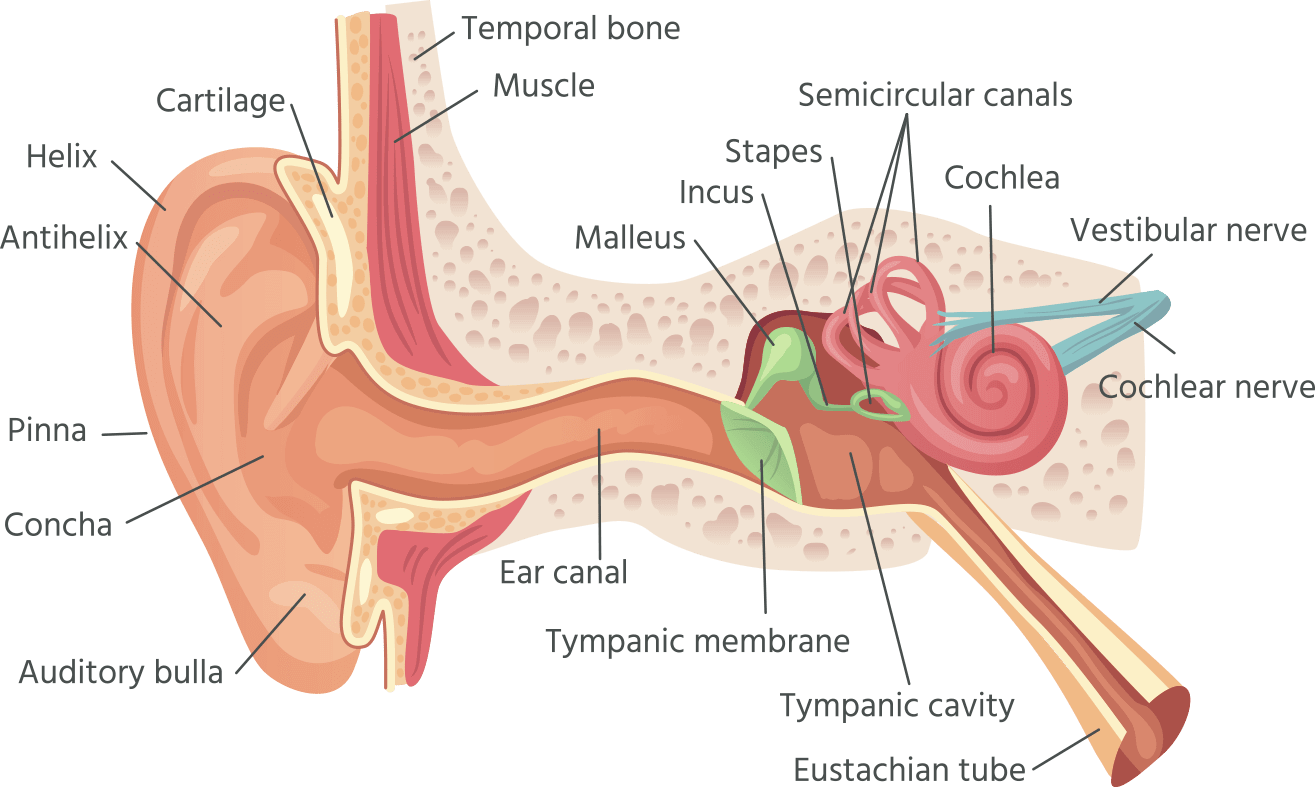
Now that we know what types of hearing aids there are, let's talk about hearing anatomy; it will help you better understand what causes hearing loss and how to address it. The human hearing system has four parts:
- The outer ear collects, directs, and amplifies incoming sound. This part of the ear includes the Pinna (where you hang your glasses), the ear canal, and the outer surface of the eardrum (tympanic membrane).
- The middle ear is a mechanical amplifier. Behind the eardrum, the three smallest bones in the body: the hammer, anvil, and stirrup (or malleus, incus, and stapes for you Latin fans) amplify the sound energy in the ear canal; they also deliver those enhanced vibrations to the inner ear. Collectively, these bones are known as ossicles. An often neglected part of the middle ear is the Eustachian tube. This structure connects the middle ear to the back of the nose and allows your ears to “pop” on an airplane or when scuba diving.
- The inner ear includes the cochlea and the vestibular, or balance system. The cochlea contains roughly 30,000 tiny receptors called hair cells; these receptors convert the vibrations in the cochlear fluid into nerve impulses. The inner ear’s balance components convert movement into nerve impulses.
- The central auditory system is the “computer” of hearing. It includes a sophisticated group of structures in the auditory nerve, brain stem, and several areas of the brain. These brain areas decode nerve impulses from the inner ear into perceptions of pitch, loudness, and duration. This system combines with memory to allow us to hear and understand speech and other sounds.
Causes and Types of Hearing Loss
The type of hearing loss you have determines the kind of hearing aid your audiologist will recommend to you.
Hearing loss can refer to the inability to hear volume accurately, AKA “hearing sensitivity.” Hearing loss can also refer to the inability to hear sounds accurately within specific frequencies; it's called “hearing discrimination.”3
We separate hearing ability into which parts of the hearing mechanism are affected (type of loss), plus how loud sounds need to be for you to hear (severity of loss).
- Conductive hearing loss results from reduced function of the outer or middle ear. This decline generally affects sensitivity (the world gets quieter) but not discrimination (making things louder improves understanding). Conductive hearing loss in adults accounts for roughly 5 to 15 percent of hearing loss and is generally treatable medically.
- Sensorineural hearing loss involves dysfunction of the cochlea or auditory nerve. It accounts for approximately 90 percent of hearing loss in adults. Sensorineural hearing loss is sometimes called acquired hearing loss since it occurs after birth (you're not born with it). Sensorineural hearing loss can be caused by damage to the inner ear (cochlea) or to the nerve pathways that transmit sound to the brain.5 It results from various issues, including aging, loud noise exposure, or taking ototoxic drugs (medications or medical treatments that negatively impact hearing). As an audiologist, I look at acquired hearing loss based on which parts of the inner ear are likely affected.6
Facts and Statistics About Hearing Loss
- Globally, 430 million people have disabling hearing loss.6
- Hearing loss is the third most common physical condition behind arthritis and heart disease.7
- Roughly 33 percent of people over 65 have hearing loss.8
- Mild hearing loss doubles dementia risk. That risk increases consistently with hearing loss
- Hearing loss can also lead to depression, increasing the risk of falls in older adults.
- Across the globe, only 17 percent of those who need a hearing aid use
- Older adults who use hearing aids have reduced signs of depression and an improved quality of life.
How to Know If You Have Hearing Loss: Tests and Evaluations
Now that we know a little about what might cause hearing to degrade, let’s talk about how to find out if your hearing isn’t up to snuff.
People with hearing loss tend to exhibit or notice one or more of these behaviors:
- Asking people to repeat themselves, particularly in settings with background noise (restaurants, stores, offices, etc.)
- Listening to television or other media at a louder volume than family or friends
- Avoiding social situations that require listening (meetings, houses of worship, parties, etc.)
- Missing the punch lines of jokes
- A decreasing level of confidence that you understand what people say
- Monopolizing conversations to avoid having to hear and understand other people
- You've started to notice tinnitus sounds, like humming, ringing, or buzzing, in one or both ears
In the video below, I further discuss how to spot the early signs of hearing loss with SeniorLiving.org's Editor-in-Chief, Jeff Hoyt.
If you do any of these things more often than you change the oil in your car, you should have your hearing evaluated. There are two basic forms of checking out your hearing: a screening and an evaluation.
Hearing Screenings and How They Work
A hearing screening is used to determine if hearing loss likely exists. It's not a diagnostic test, and it won't identify the specific type of hearing loss you may have or its likely cause.
These types of tests generally only address the sensitivity part of hearing. They're quick and typically free. Like other types of health screenings, a hearing screening lets you know if further investigation is needed. Hearing tests are available in many apps and websites where hearing aids are sold. You can also use SeniorLiving.org's online screening test as a first step.
A hearing care professional may also recommend a type of test called a pure-tone audiometric screening. These are identical to your hearing test in the nurse’s office in elementary school. Like smartphone apps, they offer insight into your hearing abilities and indicate if further testing is warranted.
They may also recommend a speech discrimination test. This type of test analyzes your ability to clearly hear and discern speech. Presbycusis — age-related hearing loss — often begins with reduced higher-frequency hearing ability. This test helps sleuth that out.
Hearing Evaluation
If your hearing screening suggests that you may have hearing loss, it’s best to have a complete hearing evaluation. That can be performed by either an audiologist or a licensed hearing instrument specialist.
Your hearing evaluation will include several tests, including:
- Visual inspection of the inner and outer ear
- Evaluation of middle-ear function
- Pure-tone testing to identify the softest sounds you hear at each pitch
- Bone-conduction testing to look for wax or fluid buildup
- Speech testing
- Auditory brainstem response to analyze the efficacy of the communication pathways between the inner ear and the brain
- Otoacoustic emissions test to check inner ear function
- Tympanometry to analyze eardrum movements

Audiologist Dr. Ruth Reisman demonstrates taking a hearing evaluation
What to Expect During Your First Audiologist Visit Video
Making an appointment to visit the doctor can be stressful, but your first audiologist visit doesn't have to be! Audiologists are trained professionals who specialize in hearing and the ear. They can provide you with a thorough assessment of your hearing loss. Things will be crystal clear in terms of your hearing and your knowledge of your ears by the end. Watch the video below to learn what to expect during your first audiologist visit.
If I Have Hearing Loss, Do I Need a Prescription for Hearing Aids?
That depends on the level of hearing loss you have. In October 2022, new legislation was passed that allows hearing aids to be sold over the counter. These over-the-counter (OTC) hearing aids are designed for adults with mild to moderate hearing loss and can be purchased online or from a drug store.
There are not currently any OTC solutions available for severe to profound hearing loss; those with higher levels of hearing loss need a prescription for hearing aids suitable to their needs. Prescription hearing aids require an in-person visit to a hearing care professional to assess your hearing needs and help you find the best solution for your hearing loss.
Where to Buy Hearing Aids
There are several places to buy hearing aids, including audiology clinics, retail chains, VA medical centers, and online. Below is a complete list of where you can purchase hearing aids:
- Private-practice audiology clinics
- Otolaryngology offices
- Manufacturer-owned retail chains such as Miracle-Ear, Beltone, Audibel, Connect Hearing, and Hearing Life
- VA medical centers
- OTC retailers such as Walgreens, CVS, Walmart, Best Buy, and Hy-Vee
Adjusting Hearing Aids After Purchase
OTC Hearing Aids
If you purchase OTC hearing aids, the devices will be shipped right to your door — you won't need to visit a hearing care professional for fittings or adjustments. OTC providers typically offer remote help.
You can get all set up from the comfort of your home; however, these hearing aids aren't usually as customizable as prescription hearing aids. Some OTC hearing aids may even be preprogrammed with little to no room for adjustments.
Keep in mind that wearing hearing aids has a learning curve. Allow yourself time to adjust. In the long run, this will provide you with enhanced hearing ability and, hopefully, more enjoyment of life!
Prescription Hearing Aids
After purchasing prescription hearing aids, you need your devices fitted and programmed to your specific hearing needs in person. If you work with an audiologist, the hearing aids you select will be ordered; then, you will return for a fitting between two days and a few weeks. The audiologist will adjust your hearing aids to fit your ears and set your sound levels for optimum listening throughout multiple environments. They'll explain how to use all the programming features, such as using Bluetooth, while you drive. Of course, they'll also answer any questions you may have.
If properly fitted, hearing aids shouldn’t need many adjustments. However, it’s vital to specify precisely how many adjustment appointments come in the price and how much additional service might cost. It varies between providers, and it can represent significant ongoing costs.
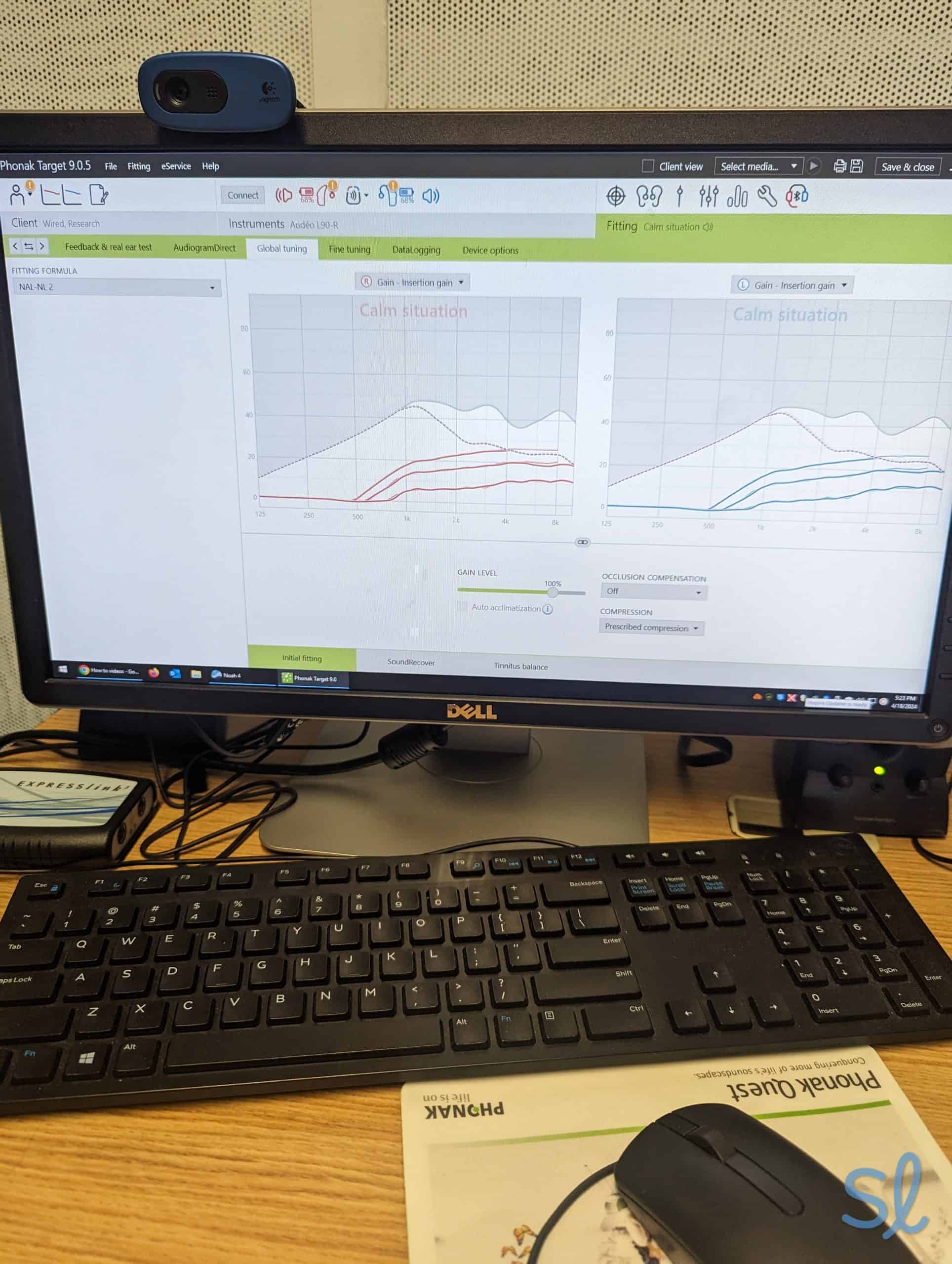
Dr. Ruth Reisman testing and customizing a pair of hearing aids
Wrapping Up
As you can see, getting hearing aids is not as simple as grabbing a pair of readers off the rack at the drugstore. Nor is it an impossible task!
Hearing is one of our primary senses because it connects us with the thoughts and emotions of those in our lives. As such, it's worth researching thoroughly, asking hard questions, and being patient to find a solution and provider that matches your needs and personality.
After the devices hit your ears, a process of neural rewiring begins that can take up to three months, so be patient. Seek the advice of others who have walked in these new and louder shoes. On the lighter side, remember that the volume control on your new hearing aids gives you the superpower of reducing the rhetoric and amplifying the awesome!
-
NIH. (2025). Hearing Aids.
-
Widex.com. (2025). DISCRIMINATION HEARING LOSS.
-
UNC School of Medicine. (n.d.). Understanding Hearing Loss.
-
WHO. (2020). Deafness and hearing loss.
-
Wexner Medical Center. (n.d.). Hearing Loss.
-
CDC. (2024). Challenges Affecting Health Literacy of Older Adults.
-
Hopkins Medicine. (n.d.). The Hidden Risks of Hearing Loss.
-
U.C. Davis. (2024). Now, hear this! Help change mindsets for World Hearing Day.